By the end of 2025, Dr Charles Pilgrim reached a significant milestone in his surgical career — more than 5,000 surgical cases performed as a consultant.
That number represents far more than volume. It reflects decades of decision-making, responsibility, refinement, and leadership across Upper Gastrointestinal surgery, robotic surgery, and bariatric surgery.
For patients, this level of experience combined with academic leadership directly influences safety, outcomes and confidence in care.
What 5,000+ Cases Really Means
Surgery is not static. No two patients are identical and no two operations are ever the same.
Across thousands of cases, a surgeon is exposed to:
- Wide anatomical variation
- Complex pathology
- Prior surgeries and scar tissue
- Unexpected findings
- Rare and high-risk scenarios
This breadth of exposure builds something that cannot be taught quickly: judgement.
With experience, surgeons develop the ability to anticipate problems, adapt in real time, and make calm, informed decisions when situations change — particularly in complex Upper GI and robotic procedures where precision is critical.
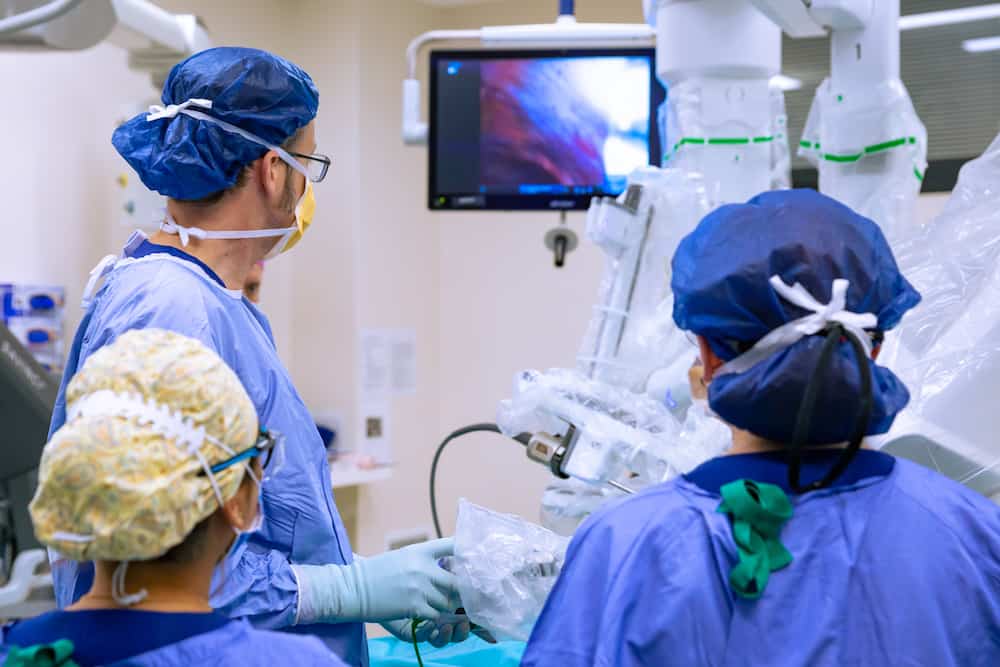

Experience Shapes Better Surgical Decisions — Before Surgery Even Begins
Highly experienced surgeons don’t just operate — they advise.
After thousands of cases, decision-making becomes more nuanced and patient-specific. Planning is informed by:
- Long-term outcomes observed over many years
- Understanding which approaches work best for which patients
- Knowing when surgery is beneficial — and when it isn’t
This matters across all Upper GI surgery, including reflux disease, hernias, cancer surgery, bariatric procedures and robotic operations. Experience allows treatment recommendations to be tailored, not templated.
Why Surgical Experience Improves Safety
No surgeon can promise zero complications. What defines excellence is how risks are managed.
Surgeons with extensive case volumes are more likely to:
- Recognise early warning signs
- Anticipate potential complications
- Intervene quickly and appropriately
In Upper GI and robotic surgery, where anatomy is complex and margins for error are small, this depth of experience plays a critical role in patient safety and recovery.
The Significance of Being an Associate Professor
Beyond clinical experience, Dr Pilgrim is an Associate Professor — a role that carries meaning well beyond the title.
Academic surgeons are expected to:
- Teach and mentor future surgeons
- Critically evaluate evidence and evolving techniques
- Contribute to surgical standards and education
This academic involvement ensures practice remains current, evidence-based, and continually refined. It also reflects peer recognition of expertise, leadership and contribution to the field.
For patients, this means their care is guided not only by experience but by ongoing engagement with best practice and surgical advancement.

Experience Across Upper GI, Robotic and Bariatric Surgery
While bariatric surgery is a key focus, Dr Pilgrim’s experience spans the full spectrum of Upper GI surgery — including advanced robotic techniques.
That breadth matters. Surgeons who work across multiple Upper GI disciplines develop a deeper understanding of anatomy, physiology, and long-term outcomes. This cross-disciplinary expertise strengthens decision-making and surgical planning, particularly for patients with complex or overlapping conditions.
What Patients Gain From This Level of Experience
More than 5,000 cases represent:
- Thousands of patient journeys
- Thousands of outcomes followed over time
- Thousands of lessons learned
For patients, it offers reassurance — that their surgeon has seen complexity, managed challenges, and refined their approach through extensive real-world experience.
Choosing a surgeon is about more than credentials or technology. It’s about trust, judgement, and leadership built over time.
In surgery, experience doesn’t just matter — it shapes everything.
